Final ID: TH891
Association of Cardiovascular and Social Risk Factors with Cognitive Function in Low Income Hypertension Patients with Low Cognitive Reserve
Abstract Body: Introduction: Increasing evidence has identified modifiable risk factors for Alzheimer’s disease and related dementias (ADRD). Yet most studies include individuals with few cardiovascular co-morbidities, high education/SES, and few racial/ethnic minorities. We analyzed relationships between modifiable risk factors and cognitive function in low-income, predominantly Black, hypertensive patients with a high burden of cardiovascular co-morbidities.
Methods: This cross-sectional analysis included 1,308 low-income, racial minority hypertensive patients in 44 low resource clinics in Louisiana, Mississippi, and Texas. ADRD risk factors included: low education (2), social contact (married or living with a partner), and self-reported prior diagnosis of diabetes, depression, and high cholesterol. Cognitive function was measured using the MoCA and a neuropsychological test battery assessing global cognitive function, executive function, and memory. Linear regression models assessed associations between each modifiable ADRD risk factor and MoCA score, standardized global cognitive, executive function, and memory scores. Models were adjusted for age, sex, race, and all other ADRD risk factors.
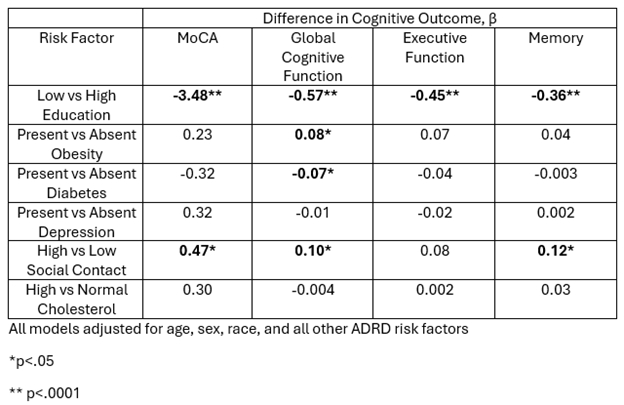
Results: Participants had a mean age of 64.5 years, 62.5% were Black, 61.3% female, and the mean MoCA score was 19.8. About 60% were obese, 46% had diabetes, and 67% had high cholesterol. Social contact was associated with higher MoCA (β=0.47, p=0.03), higher global cognitive function (β=0.10, p=0.005), and higher memory (β=0.12, p=0.0009) but not with executive function after adjustment. Low education was associated with lower MoCA (β=-3.48, p<.0001), lower global cognitive function (β=-0.57, p<.0001), lower executive function (β=-0.45, p<.0001), and lower memory (β=-0.36, p<.0001). Diabetes was associated with lower standardized global cognitive score (β=-0.07, p=0.03) but not with MoCA, executive function, or memory. Obesity was associated with higher standardized global cognitive score (β=0.08, p=0.03) but not MoCA, executive function, or memory. Depression and high cholesterol were not significantly associated with cognitive outcomes after adjustment.
Conclusions: Low education, diabetes, and less social contact were associated with lower cognitive function in understudied hypertensive patients. Targeting these factors could benefit cognition in low-income hypertensive patients with cardiovascular co-morbidities.
Methods: This cross-sectional analysis included 1,308 low-income, racial minority hypertensive patients in 44 low resource clinics in Louisiana, Mississippi, and Texas. ADRD risk factors included: low education (
Results: Participants had a mean age of 64.5 years, 62.5% were Black, 61.3% female, and the mean MoCA score was 19.8. About 60% were obese, 46% had diabetes, and 67% had high cholesterol. Social contact was associated with higher MoCA (β=0.47, p=0.03), higher global cognitive function (β=0.10, p=0.005), and higher memory (β=0.12, p=0.0009) but not with executive function after adjustment. Low education was associated with lower MoCA (β=-3.48, p<.0001), lower global cognitive function (β=-0.57, p<.0001), lower executive function (β=-0.45, p<.0001), and lower memory (β=-0.36, p<.0001). Diabetes was associated with lower standardized global cognitive score (β=-0.07, p=0.03) but not with MoCA, executive function, or memory. Obesity was associated with higher standardized global cognitive score (β=0.08, p=0.03) but not MoCA, executive function, or memory. Depression and high cholesterol were not significantly associated with cognitive outcomes after adjustment.
Conclusions: Low education, diabetes, and less social contact were associated with lower cognitive function in understudied hypertensive patients. Targeting these factors could benefit cognition in low-income hypertensive patients with cardiovascular co-morbidities.
More abstracts on this topic:
Acute Hemodynamic Effects and Synthetic Cooling Agents in “Clear” E-cigarettes Marketed in Massachusetts After the Tobacco Product Flavoring Ban
A Longitudinal 20-year Analysis Indicates Acceleration of Cardiometabolic Comorbidities on Dementia Risk
Minetti Erika, Erythropel Hanno, Keith Rachel, Davis Danielle, Zimmerman Julie, Krishnan-sarin Suchitra, Hamburg Naomi
A Longitudinal 20-year Analysis Indicates Acceleration of Cardiometabolic Comorbidities on Dementia Risk
Lihua Huang, Danish Muhammad, Auyeung Tw, Jenny Lee, Kwok Timothy, Abrigo Jill, Wei Yingying, Lo Cecilia, Fung Erik