Final ID: TU265
Temporal Trends and Demographic Disparities in Mortality Associated with Coronary Artery Disease and Sleep Disorders Among Adults in the United States: Insights from the CDC WONDER Database 1999–2020
Abstract Body: Background: Sleep disorders have been found to be associated with increased risk of Coronary Artery Disease (CAD) and lead to increased mortality. Despite that, the trends in mortality in CAD and sleep disorders remain underexplored.
Research Question: What are the temporal trends and demographic disparities in CAD mortality associated with sleep disorders among adults aged ≥25 years in the United States (U.S.)?
Aim: To analyze national trends and demographic disparities in sleep disorder–associated CAD mortality among U.S. adults from 1999 to 2020.
Methods: We analyzed the CDC WONDER database, identifying adults aged ≥25 years from 1999 to 2020, where CAD (ICD-10 I20–I25) and sleep disorders (ICD-10 G47) were listed as contributing causes of death. Age-adjusted mortality rates (AAMRs) per 100,000 were calculated and stratified by year, sex, race, region, urbanization, and state. Trends were analyzed using Joinpoint regression to calculate annual percent change (APC) and average annual percent change (AAPC).
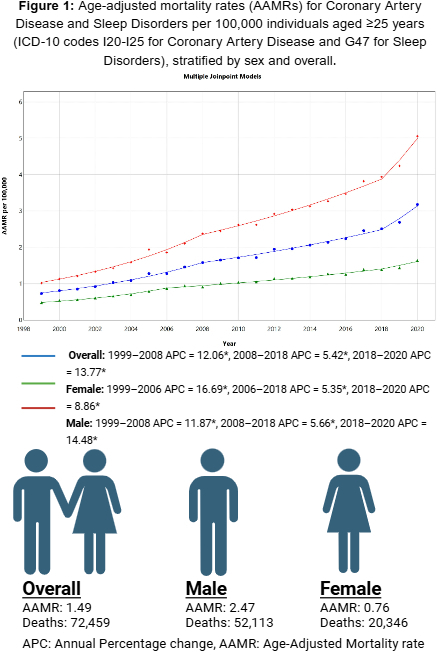
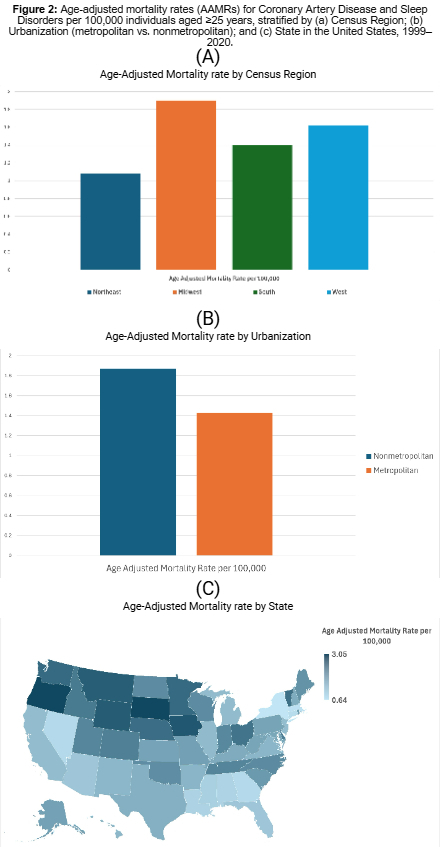
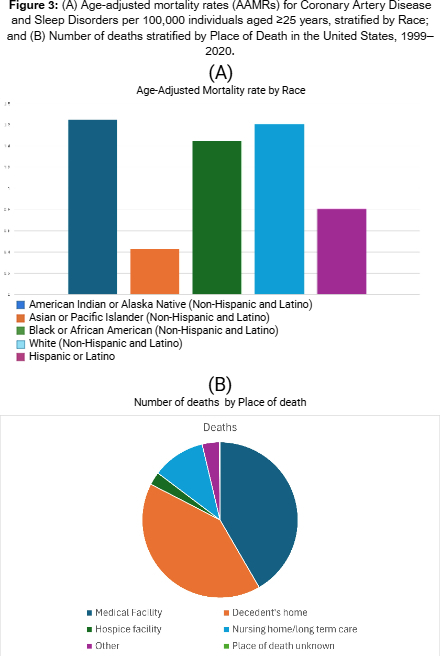
Results: From 1999 to 2020, 72,459 deaths were attributed to CAD and sleep disorders among U.S. adults aged ≥25 years. The overall AAMR increased from 0.45 in 1999 to 2.90 in 2020, with an AAPC of 9.01%. Notably, the AAMR increased sharply from 1999 to 2008 (APC 12.06, p < 0.000001), followed by a moderate increase from 2008 to 2018 (APC 5.42, p < 0.000001), and a steep increase again from 2018 to 2020 (APC 13.77, p =0.00034). AAMRs were higher in men than women (2.47 vs. 0.76), with both genders experiencing significant increases in mortality (AAPC 9.1, p <0.000001 in men vs AAPC 9.3, p < 0.000001 in women). Regionally, the Midwest recorded the highest AAMR (1.90), while the Northeast (1.08) had the lowest. Nonmetropolitan areas had higher AAMRs than metropolitan areas (1.87 vs. 1.43). By race, non-Hispanic (NH) American Indian/Alaska Natives had the highest AAMR (1.65), while NH Asian/Pacific Islanders had the lowest (0.43). State-level disparities were notable, with Oregon and South Dakota having the highest AAMRs (3.05). Most deaths occurred in medical facilities (41.6%).
Conclusion: Mortality due to sleep disorders with CAD has significantly increased from 1999 to 2020 in the U.S., disproportionately affecting men, NH American Indian/Alaska Natives, residents of nonmetropolitan areas, and the Midwest. The increasing mortality and existing disparities call for targeted intervention to improve health outcomes, especially in vulnerable populations.
Research Question: What are the temporal trends and demographic disparities in CAD mortality associated with sleep disorders among adults aged ≥25 years in the United States (U.S.)?
Aim: To analyze national trends and demographic disparities in sleep disorder–associated CAD mortality among U.S. adults from 1999 to 2020.
Methods: We analyzed the CDC WONDER database, identifying adults aged ≥25 years from 1999 to 2020, where CAD (ICD-10 I20–I25) and sleep disorders (ICD-10 G47) were listed as contributing causes of death. Age-adjusted mortality rates (AAMRs) per 100,000 were calculated and stratified by year, sex, race, region, urbanization, and state. Trends were analyzed using Joinpoint regression to calculate annual percent change (APC) and average annual percent change (AAPC).
Results: From 1999 to 2020, 72,459 deaths were attributed to CAD and sleep disorders among U.S. adults aged ≥25 years. The overall AAMR increased from 0.45 in 1999 to 2.90 in 2020, with an AAPC of 9.01%. Notably, the AAMR increased sharply from 1999 to 2008 (APC 12.06, p < 0.000001), followed by a moderate increase from 2008 to 2018 (APC 5.42, p < 0.000001), and a steep increase again from 2018 to 2020 (APC 13.77, p =0.00034). AAMRs were higher in men than women (2.47 vs. 0.76), with both genders experiencing significant increases in mortality (AAPC 9.1, p <0.000001 in men vs AAPC 9.3, p < 0.000001 in women). Regionally, the Midwest recorded the highest AAMR (1.90), while the Northeast (1.08) had the lowest. Nonmetropolitan areas had higher AAMRs than metropolitan areas (1.87 vs. 1.43). By race, non-Hispanic (NH) American Indian/Alaska Natives had the highest AAMR (1.65), while NH Asian/Pacific Islanders had the lowest (0.43). State-level disparities were notable, with Oregon and South Dakota having the highest AAMRs (3.05). Most deaths occurred in medical facilities (41.6%).
Conclusion: Mortality due to sleep disorders with CAD has significantly increased from 1999 to 2020 in the U.S., disproportionately affecting men, NH American Indian/Alaska Natives, residents of nonmetropolitan areas, and the Midwest. The increasing mortality and existing disparities call for targeted intervention to improve health outcomes, especially in vulnerable populations.
More abstracts on this topic:
Multidimensional Association Of Sleep With Health Behaviors and Cardiometabolic Risk In AdolescentsMultidimensional Association Of Sleep With Health Behaviors and Cardiometabolic Risk In Adolescents
Nyhuis Casandra, Fernandez-mendoza Julio, Morales-ghinaglia Natasha, Rahawi Anthony, Ballester-navarro Pura, Calhoun Susan, Liao Jason, Vgontzas Alexandros, Liao Duanping, Bixler Edward
Prevalence and Prognostic Implications of Sleep Disordered Breathing in Hypertrophic CardiomyopathyKarim Shahid, Geske Jeffrey, Somers Virend, Chahal Anwar, Venkataraman Shreyas, Deshmukh Abhishek, Siontis Konstantinos, Mansukhani Meghna, Konecny Thomas, Khanji Mohammed, Petersen Steffen