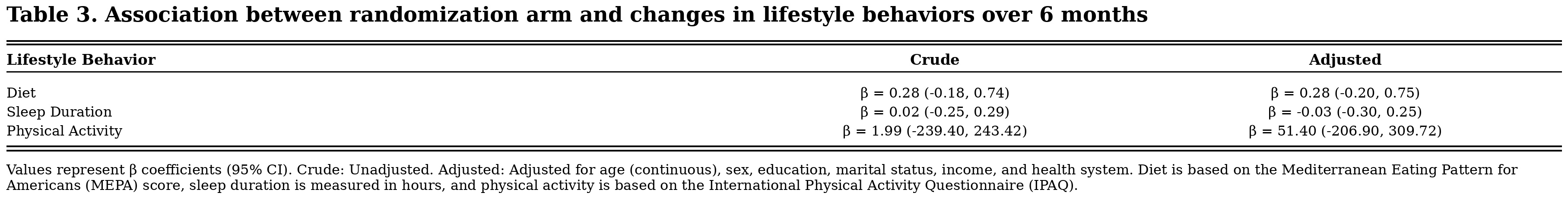Final ID: MPTH66
No Significant Six-Month Changes in Lifestyle Behaviors Among Adults with Elevated BP or Stage 1 Hypertension in the LINKED-BP Program
Abstract Body: Background: Lifestyle modification is central to hypertension prevention and control. Despite its recognized importance, few community-based clinical trials have evaluated short-term behavioral change within multicomponent interventions.
Objective: To examine six-month changes in diet, sleep, and physical activity, among adults in a hypertension prevention trial [Home Blood Pressure Telemonitoring LINKED with CHWs to Improve Blood Pressure(LINKED-BP) Program (NCT05719647)] randomized to a multilevel intervention versus enhanced usual care. We hypothesized that participants in the intervention arm would have greater improvements in these lifestyle behaviors than those in the control arm.
Methods: Participants were adults aged ≥18 years at risk for stage 2 hypertension who were enrolled in the LINKED-BP Program. This cluster randomized clinical trial was conducted across health systems in Maryland and the Washington, DC metropolitan area. Participants were randomized to a multi-level intervention with community health workers providing education and lifestyle modification support or enhanced usual care over a 12-month period. For this analysis, we included participants with baseline and 6-month survey data. We assessed six-month changes in diet (Mediterranean Eating Pattern for Americans score), nightly sleep duration (hours), and physical activity (International Physical Activity Questionnaire). Descriptive statistics and multivariable linear regression were used to analyze the association between study arm and changes in lifestyle behaviors.
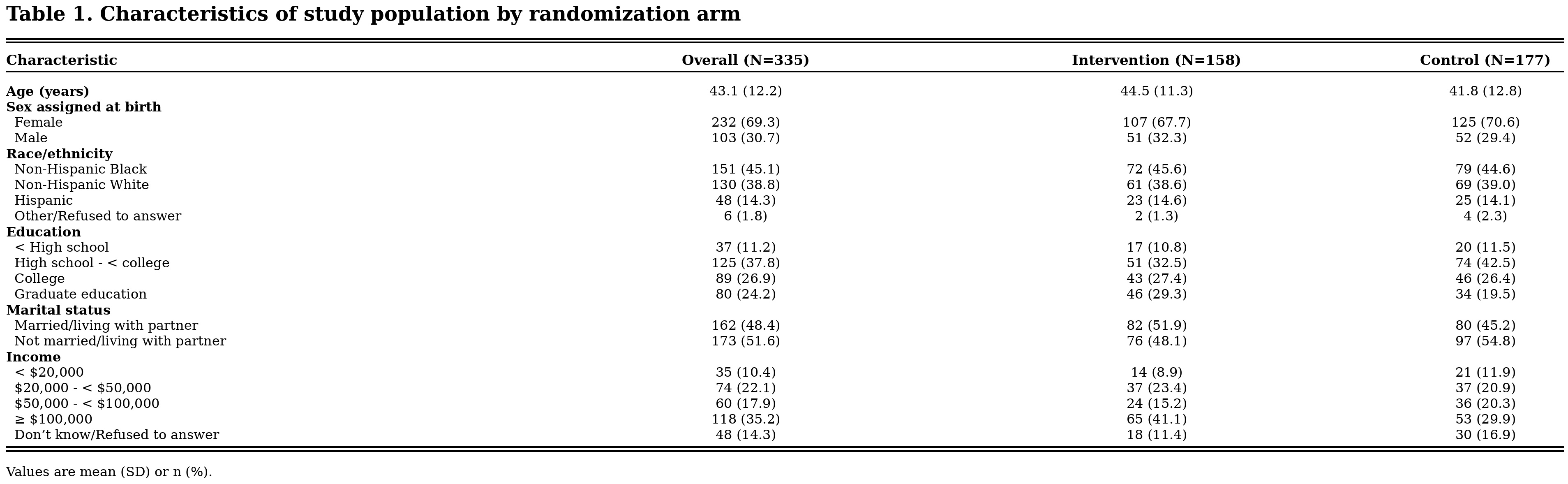
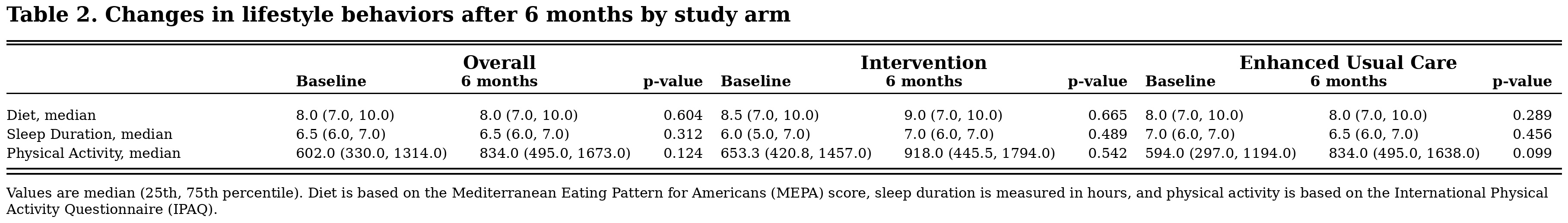
Results: Participants (N=335) had a mean age of 43.1 (± 12.2) years and 69% were female (Table 1). Between baseline and 6 months, physical activity increased modestly across both groups (602 to 834 MET-min/week overall), but the change was not statistically significant (Table 2). Other lifestyle behaviors remained largely unchanged. Multi-variable adjusted models comparing the intervention with enhanced usual care showed no significant between-group differences in the changes in diet (0.28 [–0.20, 0.75]), sleep (–0.03 [–0.30, 0.25]), or physical activity (51.4 [–206.9, 309.7]) (Table 3).
Conclusions: Preliminary data from this cluster-randomized trial showed non-significant within-group improvements in physical activity over 6 months. Achieving meaningful behavioral change in real-world hypertension management may require more intensive, sustained, and equity-focused interventions.
Objective: To examine six-month changes in diet, sleep, and physical activity, among adults in a hypertension prevention trial [Home Blood Pressure Telemonitoring LINKED with CHWs to Improve Blood Pressure(LINKED-BP) Program (NCT05719647)] randomized to a multilevel intervention versus enhanced usual care. We hypothesized that participants in the intervention arm would have greater improvements in these lifestyle behaviors than those in the control arm.
Methods: Participants were adults aged ≥18 years at risk for stage 2 hypertension who were enrolled in the LINKED-BP Program. This cluster randomized clinical trial was conducted across health systems in Maryland and the Washington, DC metropolitan area. Participants were randomized to a multi-level intervention with community health workers providing education and lifestyle modification support or enhanced usual care over a 12-month period. For this analysis, we included participants with baseline and 6-month survey data. We assessed six-month changes in diet (Mediterranean Eating Pattern for Americans score), nightly sleep duration (hours), and physical activity (International Physical Activity Questionnaire). Descriptive statistics and multivariable linear regression were used to analyze the association between study arm and changes in lifestyle behaviors.
Results: Participants (N=335) had a mean age of 43.1 (± 12.2) years and 69% were female (Table 1). Between baseline and 6 months, physical activity increased modestly across both groups (602 to 834 MET-min/week overall), but the change was not statistically significant (Table 2). Other lifestyle behaviors remained largely unchanged. Multi-variable adjusted models comparing the intervention with enhanced usual care showed no significant between-group differences in the changes in diet (0.28 [–0.20, 0.75]), sleep (–0.03 [–0.30, 0.25]), or physical activity (51.4 [–206.9, 309.7]) (Table 3).
Conclusions: Preliminary data from this cluster-randomized trial showed non-significant within-group improvements in physical activity over 6 months. Achieving meaningful behavioral change in real-world hypertension management may require more intensive, sustained, and equity-focused interventions.
More abstracts on this topic:
2 Dimensional Echocardiography versus 3 Dimentional Echocardiography to Assess Right Ventricular Function in Pulmonary Hypertension: A Systematic Review
Chaudhry Waleed Razzaq, Hajj Fatima, Bathula Satyamedha, Meghji Mohammed Askari, Pasupuleti Hemalatha, Kiyani Madiha, Shah Syeda Simrah, Neelakantan Ramaswamy Sanathanan, Mirzaeidizaji Nakisa, St. Jacques Jahnoy, Khan Khalil Ullah, Veluchamy Elakkiya, Jesse Joshanna
An evaluation of a visual arts-based intervention for promoting psychosocial functioning of community-dwelling stroke survivors: A randomized controlled trialChan Mimi Wai Man, Lo Suzanne, Sit Janet