Final ID: WE473
Comparing Cardiac Function between South Asians in MASALA and MESA subgroups
Abstract Body: Background: Early heart failure (HF), which represents the transition from Stage B (structural/functional myocardial abnormalities only) to Stage C (symptomatic) HF, is influenced by metabolic risk factors, and may vary by ethnic ancestry. There are few normative data of cardiac structure/function among South Asian populations globally, though these populations have a disproportionately high risk of cardiovascular disease.
Research Question: Are there differences in indices of cardiac structure/function among U.S. South Asians, Whites, Blacks, Latinos, and Chinese Americans?
Methods: We used data from 785 participants in the Mediators of Atherosclerosis in South Asians Living in America (MASALA) study who completed Exam 3 (2021-2024) and 2,890 participants from the Multi-Ethnic Study of Atherosclerosis (MESA) study who completed Exam 6 (2018-2020). All participants underwent clinical and laboratory data collection, including the Kansas City Cardiomyopathy Questionnaire, a 6-minute walk test, and identical echo protocols (at rest and with passive leg raise). We age-restricted the MASALA sample to be similar to the older MESA participants (59-89 years of age, n=595). We compared cardiac function and other measures of functional status among the five race-ethnic subgroups after adjusting for age, gender, education, body mass index, waist circumference, hypertension, diabetes, and estimated GFR.
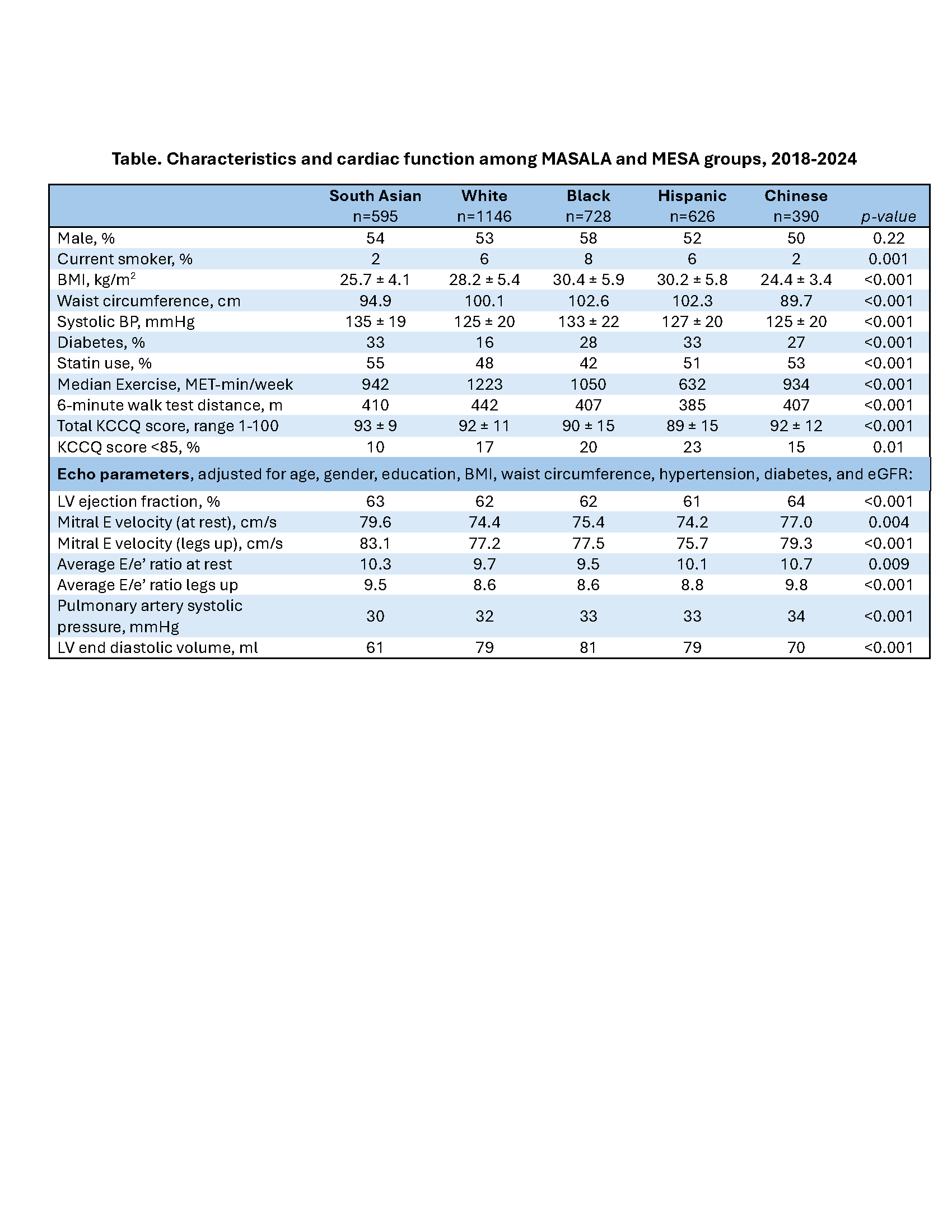
Results: Mean age was 73±8 years for MESA and 69±7 years for MASALA, and men had somewhat higher representation than women across all race/ethnic subgroups. The Table shows characteristics for MASALA participants compared to each of the four MESA groups. South Asian participants were less likely to smoke, had higher systolic blood pressure, diabetes prevalence, statin use, and KCCQ scores (indicating very few heart failure symptoms) compared to MESA groups. After multivariable adjustment, South Asians had evidence of higher mitral E velocity, high E/e’ ratio, and lowest LV end diastolic volume, which together suggest reduced LV diastolic chamber compliance, compared to all other groups.
Conclusions: South Asian populations may have a higher burden of diastolic dysfunction than other race/ethnic groups despite a lack of typical symptoms. Future investigations should determine whether better control of metabolic risk factors can improve cardiac function in all groups.
Research Question: Are there differences in indices of cardiac structure/function among U.S. South Asians, Whites, Blacks, Latinos, and Chinese Americans?
Methods: We used data from 785 participants in the Mediators of Atherosclerosis in South Asians Living in America (MASALA) study who completed Exam 3 (2021-2024) and 2,890 participants from the Multi-Ethnic Study of Atherosclerosis (MESA) study who completed Exam 6 (2018-2020). All participants underwent clinical and laboratory data collection, including the Kansas City Cardiomyopathy Questionnaire, a 6-minute walk test, and identical echo protocols (at rest and with passive leg raise). We age-restricted the MASALA sample to be similar to the older MESA participants (59-89 years of age, n=595). We compared cardiac function and other measures of functional status among the five race-ethnic subgroups after adjusting for age, gender, education, body mass index, waist circumference, hypertension, diabetes, and estimated GFR.
Results: Mean age was 73±8 years for MESA and 69±7 years for MASALA, and men had somewhat higher representation than women across all race/ethnic subgroups. The Table shows characteristics for MASALA participants compared to each of the four MESA groups. South Asian participants were less likely to smoke, had higher systolic blood pressure, diabetes prevalence, statin use, and KCCQ scores (indicating very few heart failure symptoms) compared to MESA groups. After multivariable adjustment, South Asians had evidence of higher mitral E velocity, high E/e’ ratio, and lowest LV end diastolic volume, which together suggest reduced LV diastolic chamber compliance, compared to all other groups.
Conclusions: South Asian populations may have a higher burden of diastolic dysfunction than other race/ethnic groups despite a lack of typical symptoms. Future investigations should determine whether better control of metabolic risk factors can improve cardiac function in all groups.
More abstracts on this topic:
Adipocyte-Derived Small Extracellular Vesicles Enriched with NNMT Inhibit Angiogenesis Post-Myocardial Infarction in Diabetes
Ren Hang, Cao Liwen, Zhao Zhenkun, Huang Ying, Pan Zhongjing, Cheng Liangfen, Gan Lu
A Two-Hit HFpEF-like Mouse Model with Accelerated Disease OnsetNehra Sarita, Selvam Sabariya, Anand Amit, Luettgen Joseph, Gulia Jyoti, Dokania Manoj, Gupta Ankit, Garcia Ricardo, Dudhgaonkar Shailesh, Mazumder Tagore Debarati, Ck Neethu, Wagh Somnath, Kale Prajakta