Final ID: TH888
Do Midlife Diet and Physical Activity Build Cognitive Reserve for Later Life? Results from the Framingham Heart Study
Abstract Body: Background: Physical activity (PA) and healthy dietary patterns are associated with reduced risk of cognitive decline and dementia. However, it remains unclear whether these lifestyle factors, assessed in midlife, confer greater resilience to late-life neurodegeneration on cognitive function (i.e., cognitive reserve).
Methods: We included 581 Framingham Heart Study Offspring cohort participants who completed food frequency questionnaires (FFQ) and PA questionnaires between ages 40-59 years and at least one neuropsychological (NP) assessment and brain MRI between ages 65-75 years. Dietary Approaches to Stop Hypertension (DASH) scores were based on FFQs. PA was based on the physical activity index (PAI) score. We used previously derived factor scores for memory (MEM) and executive functioning (EF) from the NP exams. MRI measures included hippocampal volume (HCV) and total brain volume (TBV). We used linear regression models to examine the two-way interaction between DASH quartiles or PAI tertiles and each outcome. Post-estimation marginal effects of the associations for each DASH group or PAI group were also obtained.
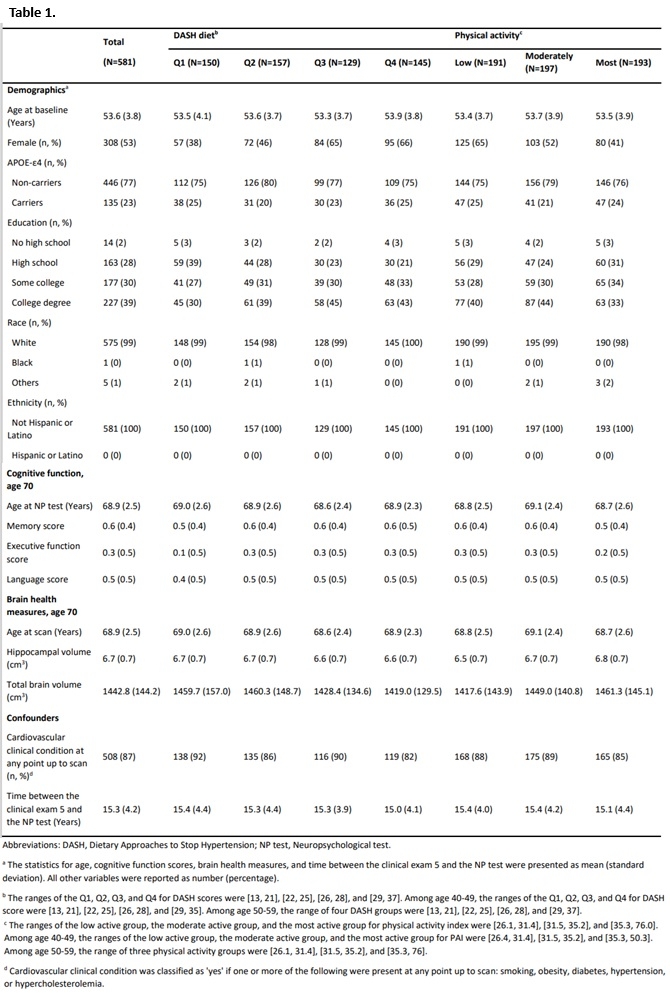
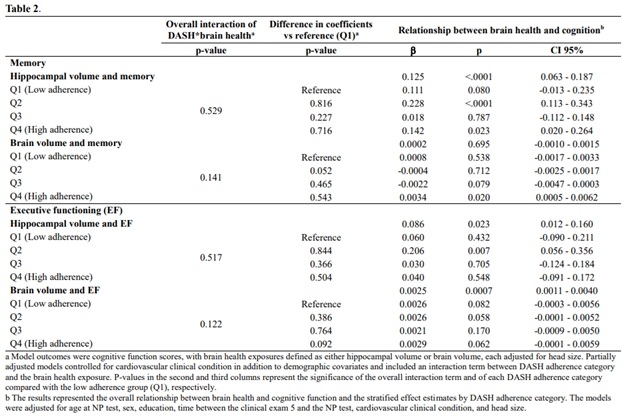
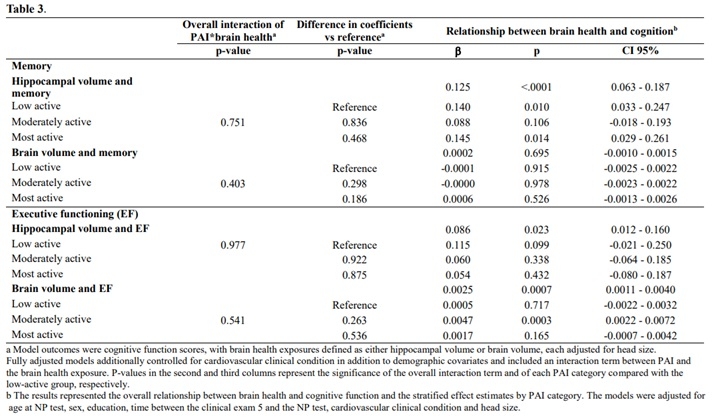
Results: Participants were on average 54 years old at baseline; 53% were female (Table 1). Relationships between brain and cognitive measures with diet and PA did not show consistent effects. For example, HCV was positively associated with MEM performance only among those in the second (β: 0.23; 95% CI: 0.11, 0.34) and fourth (β: 0.14; 95% CI: 0.02, 0.26) quartiles of DASH scores (Table 2). Greater TBV was significantly associated with better MEM performance only among those in the fourth quartile of DASH diet scores (β: 0.003; 95% CI: 0.0005, 0.01). Similar positive associations were observed for HCV with EF among individuals in the second quartile of DASH diet scores. HCV was positively associated with MEM performance among those in the first (β: 0.14; 95% CI: 0.03, 0.25) and third (β: 0.14; 95% CI: 0.03, 0.26) tertiles of PAI scores (Table 3). TBV was associated with EF only in individuals in the second tertile of PAI. No significant interactions were observed between DASH or PA and brain volume on performance in MEM and EF.
Conclusion: DASH diet or PA in midlife does not appear to confer resilience to neurodegeneration in MEM or EF at an average age of 69 years. Continued follow-up of these participants as they enter a period of greater risk for dementia may reveal effects of midlife diet and PA on cognitive resilience in later life.
Methods: We included 581 Framingham Heart Study Offspring cohort participants who completed food frequency questionnaires (FFQ) and PA questionnaires between ages 40-59 years and at least one neuropsychological (NP) assessment and brain MRI between ages 65-75 years. Dietary Approaches to Stop Hypertension (DASH) scores were based on FFQs. PA was based on the physical activity index (PAI) score. We used previously derived factor scores for memory (MEM) and executive functioning (EF) from the NP exams. MRI measures included hippocampal volume (HCV) and total brain volume (TBV). We used linear regression models to examine the two-way interaction between DASH quartiles or PAI tertiles and each outcome. Post-estimation marginal effects of the associations for each DASH group or PAI group were also obtained.
Results: Participants were on average 54 years old at baseline; 53% were female (Table 1). Relationships between brain and cognitive measures with diet and PA did not show consistent effects. For example, HCV was positively associated with MEM performance only among those in the second (β: 0.23; 95% CI: 0.11, 0.34) and fourth (β: 0.14; 95% CI: 0.02, 0.26) quartiles of DASH scores (Table 2). Greater TBV was significantly associated with better MEM performance only among those in the fourth quartile of DASH diet scores (β: 0.003; 95% CI: 0.0005, 0.01). Similar positive associations were observed for HCV with EF among individuals in the second quartile of DASH diet scores. HCV was positively associated with MEM performance among those in the first (β: 0.14; 95% CI: 0.03, 0.25) and third (β: 0.14; 95% CI: 0.03, 0.26) tertiles of PAI scores (Table 3). TBV was associated with EF only in individuals in the second tertile of PAI. No significant interactions were observed between DASH or PA and brain volume on performance in MEM and EF.
Conclusion: DASH diet or PA in midlife does not appear to confer resilience to neurodegeneration in MEM or EF at an average age of 69 years. Continued follow-up of these participants as they enter a period of greater risk for dementia may reveal effects of midlife diet and PA on cognitive resilience in later life.
More abstracts on this topic:
A Comparative Study Of Social Determinants, Hypertension, And Life Essential Factors In Alabama And Colorado From The 2021 Behavioral Risk Factor Surveillance System
Chukwunyere Chibuike, Owuor Kevin
Adoptive transfer of placental CD4+ T Cells from preeclamptic patients with a history of COVID-19 causes hypertension and cognitive dysfunction postpartum in a pregnant rat model of preeclampsiaDeer Evangeline, Simmons Kimberly, Herrock Owen, Campbell Nathan, Roman Richard, Zheng Baoying, Morris Rachael, Lamarca Babbette