Final ID: TH829
Physician Perspectives and Barriers to Tirzepatide Use in Heart Failure with Preserved Ejection Fraction and Obesity
Abstract Body: Background: The SUMMIT trial showed that Tirzepatide (TZP) reduces cardiovascular deaths or worsening heart failure (HF) events and improves quality of life in adults with heart failure with preserved ejection fraction (HFpEF) and obesity, supporting incretin-based therapy as a disease-modifying approach. Despite these findings, adoption in clinical practice may be limited due to prescriber concerns, knowledge gaps, and system-level barriers.
Methods: Cross-sectional REDCap surveys were sent to physicians across different training levels (N=60) at an academic medical center. Items assessed included experience prescribing GLP-1 receptor agonists (GLP-1 RAs) for any indication, familiarity with SUMMIT trial results, provider confidence, perceived effectiveness of TZP for patients with HFpEF and obesity, and barriers to prescription.
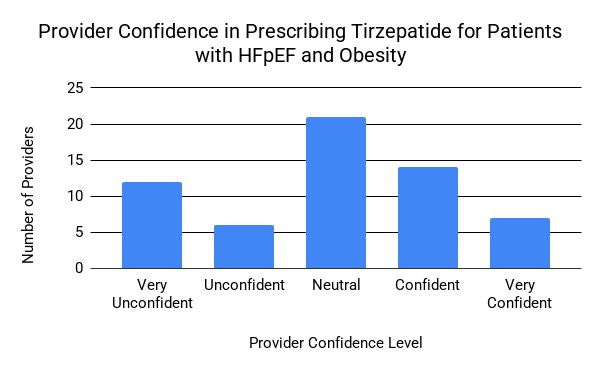
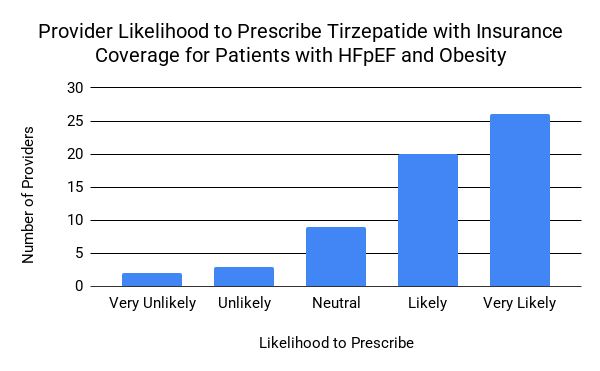
Results: Respondents were internal medicine residents (65.0%) and attendings (35.0%), all with HF management experience. Most (61.7%) had prescribed GLP-1 RAs, but only 43.3% for HFpEF and obesity. Knowledge gaps were noted, with 40.0% aware of the SUMMIT trial and 33.3% having formal GLP-1 RA training. Confidence varied: 50.0% felt confident or very confident prescribing GLP-1 RAs for any indication, decreasing to 35.0% for HFpEF and obesity. Perceived effectiveness was reflected by 58.4% rating TZP very effective and 60.0% indicating it could substantially improve quality of life. Safety perceptions of TZP consisted of 76.6% viewing the benefits outweighing the risks and would likely prescribe it if covered by insurance. The majority of respondents cited financial and insurance barriers (85.0%); more specifically, 88.2% reported high out-of-pocket costs and 86.3% identified lack of coverage or high co-pays. Other barriers included provider knowledge (40.0%), institutional logistics (25.0%), clinical concerns (23.3%), and patient factors (16.7%).
Conclusion: Our findings demonstrate that physicians recognize TZP as an effective, safe intervention for managing HFpEF and obesity. However, prescribing TZP remains constrained by financial barriers, coverage gaps, and knowledge deficits. High out-of-pocket costs highlight systemic inequities, while rapidly emerging data has outpaced clinical guidelines, resulting in inconsistent workflows. To address these challenges, we propose targeted educational initiatives on TZP use in select patients, coupled with institutional pathways to streamline prior authorization and insurance approval.
Methods: Cross-sectional REDCap surveys were sent to physicians across different training levels (N=60) at an academic medical center. Items assessed included experience prescribing GLP-1 receptor agonists (GLP-1 RAs) for any indication, familiarity with SUMMIT trial results, provider confidence, perceived effectiveness of TZP for patients with HFpEF and obesity, and barriers to prescription.
Results: Respondents were internal medicine residents (65.0%) and attendings (35.0%), all with HF management experience. Most (61.7%) had prescribed GLP-1 RAs, but only 43.3% for HFpEF and obesity. Knowledge gaps were noted, with 40.0% aware of the SUMMIT trial and 33.3% having formal GLP-1 RA training. Confidence varied: 50.0% felt confident or very confident prescribing GLP-1 RAs for any indication, decreasing to 35.0% for HFpEF and obesity. Perceived effectiveness was reflected by 58.4% rating TZP very effective and 60.0% indicating it could substantially improve quality of life. Safety perceptions of TZP consisted of 76.6% viewing the benefits outweighing the risks and would likely prescribe it if covered by insurance. The majority of respondents cited financial and insurance barriers (85.0%); more specifically, 88.2% reported high out-of-pocket costs and 86.3% identified lack of coverage or high co-pays. Other barriers included provider knowledge (40.0%), institutional logistics (25.0%), clinical concerns (23.3%), and patient factors (16.7%).
Conclusion: Our findings demonstrate that physicians recognize TZP as an effective, safe intervention for managing HFpEF and obesity. However, prescribing TZP remains constrained by financial barriers, coverage gaps, and knowledge deficits. High out-of-pocket costs highlight systemic inequities, while rapidly emerging data has outpaced clinical guidelines, resulting in inconsistent workflows. To address these challenges, we propose targeted educational initiatives on TZP use in select patients, coupled with institutional pathways to streamline prior authorization and insurance approval.
More abstracts on this topic:
Advancing Age, ASA Class, Sex, Functional Status, and Comorbidities as Predictors of Perioperative Cardiac Arrest Following Total Hip Arthroplasty: A National Cohort Study
Hussain Abdur-rehman, Soni Ashesh, Stead Thor, Persaud Nadiya, Ganti Latha
A Case Presentation of Severe Left Ventricular Dysfunction from Focal Myocarditis due to Immune Checkpoint InhibitorPatel Romil, Hussain Kifah, Gordon Robert