Final ID: 070
The Risk of Arrhythmias and Sudden Cardiac Arrest Associated with Methamphetamine, Cocaine, Opiate, and Cannabis Use: An Analysis of a Large Healthcare Claims Database
Abstract Body: Introduction: Arrhythmogenic risks associated with substance use are poorly understood; existing studies are limited in scope or conducted in select populations. We conducted a longitudinal analysis to quantify the association of substance use with incident arrhythmias and sudden cardiac arrest (SCA) in a commercially insured population in the US.
Methods: Using data from the MarketScan databases (2016-2022), we used ICD-10 codes to identify substances, outcomes, and covariates at each medical encounter. Substance users were matched with up to five non-substance users by age, sex, insurance enrollment date, and encounter date. Outcomes included atrial fibrillation (AF), ventricular tachycardia (VT), and a combined SCA/ventricular fibrillation (SCA/VF) outcome. We used Cox proportional hazards models to assess the association of each substance with each incident outcome, adjusting for demographics and comorbidities.
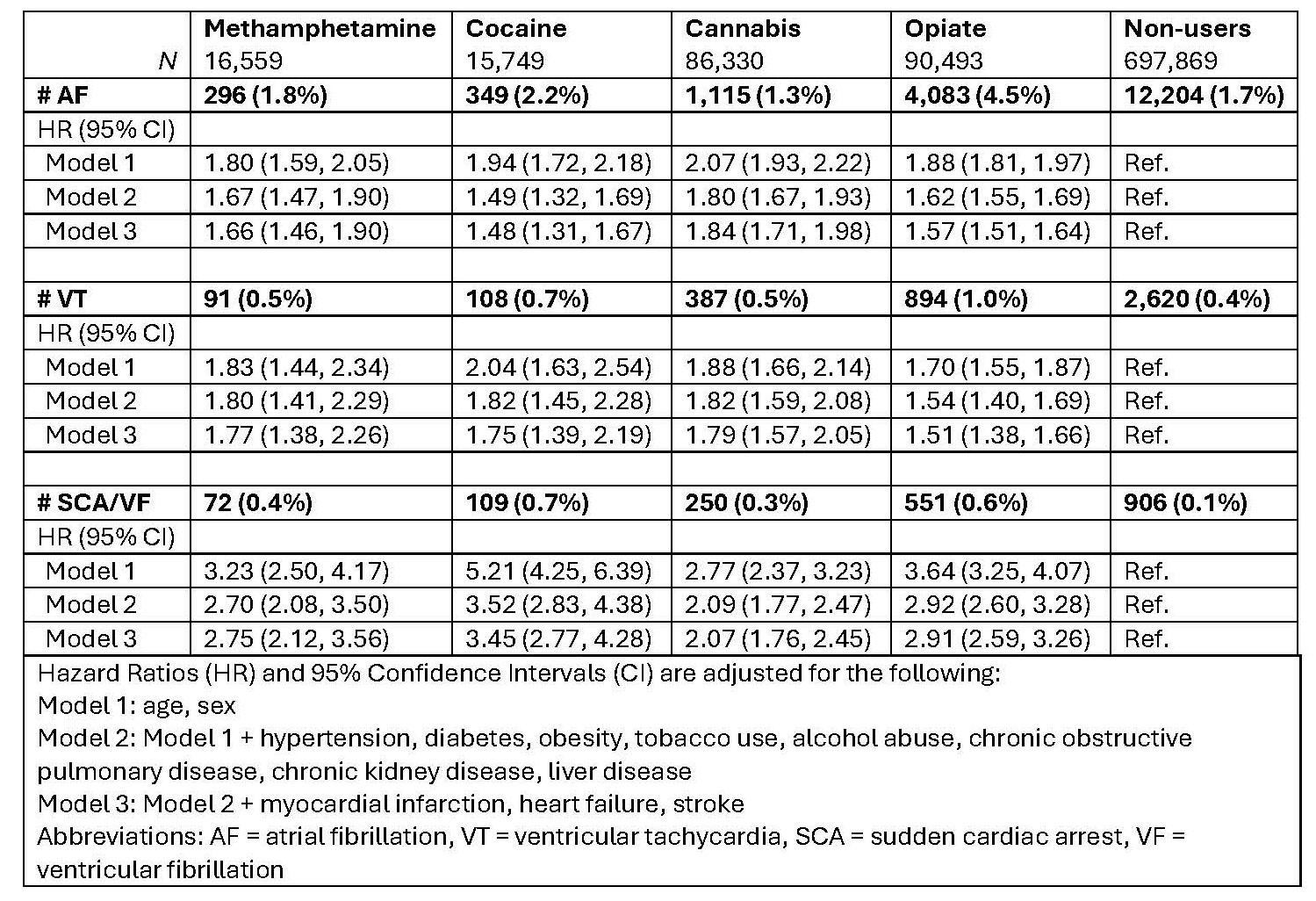
Results: We matched 154,208 substance users to 697,869 non-users (mean age = 43 years; 46% female). Opiate and cannabis use were the most common (Table). During a mean follow-up of 2.1 years, there were 25,357 AF events, 6,351 VT events, and 2,095 SCA/VA events. After adjusting for potential confounders, the use of methamphetamines, cocaine, cannabis, and opiates was each associated with an increased risk of AF, with cannabis use having the highest risk of AF [HR: 1.84 (95% CI: 1.71, 1.98)] compared to matched non-users. All substances were associated with an increased risk of VT and SCA/VF, with cocaine use having the highest risk of SCA/VF [HR: 3.45 (95% CI: 2.77, 4.28)] compared to non-users.
Conclusion: In this representative sample of commercially insured people, methamphetamine, cocaine, cannabis, and opiate use was each associated with a 1.5-3.5 times increased risk of developing arrhythmias. Given the ongoing drug crisis and increasing cannabis use in the US, understanding the association of substance use with arrhythmia risk will help better target arrhythmia prevention in these populations.
Methods: Using data from the MarketScan databases (2016-2022), we used ICD-10 codes to identify substances, outcomes, and covariates at each medical encounter. Substance users were matched with up to five non-substance users by age, sex, insurance enrollment date, and encounter date. Outcomes included atrial fibrillation (AF), ventricular tachycardia (VT), and a combined SCA/ventricular fibrillation (SCA/VF) outcome. We used Cox proportional hazards models to assess the association of each substance with each incident outcome, adjusting for demographics and comorbidities.
Results: We matched 154,208 substance users to 697,869 non-users (mean age = 43 years; 46% female). Opiate and cannabis use were the most common (Table). During a mean follow-up of 2.1 years, there were 25,357 AF events, 6,351 VT events, and 2,095 SCA/VA events. After adjusting for potential confounders, the use of methamphetamines, cocaine, cannabis, and opiates was each associated with an increased risk of AF, with cannabis use having the highest risk of AF [HR: 1.84 (95% CI: 1.71, 1.98)] compared to matched non-users. All substances were associated with an increased risk of VT and SCA/VF, with cocaine use having the highest risk of SCA/VF [HR: 3.45 (95% CI: 2.77, 4.28)] compared to non-users.
Conclusion: In this representative sample of commercially insured people, methamphetamine, cocaine, cannabis, and opiate use was each associated with a 1.5-3.5 times increased risk of developing arrhythmias. Given the ongoing drug crisis and increasing cannabis use in the US, understanding the association of substance use with arrhythmia risk will help better target arrhythmia prevention in these populations.
More abstracts on this topic:
Blocking CCN1/α6β1 axis attenuates Angiotensin II-induced aortic aneurysms in mice
Lee Tsai-jung, Mo Fan
Automated Personalized Modulation of the Sympathetic “fight-or-flight” Reflex In Vivo Using Implantable Microdevices for Enhancing Neurocardiac Function and Reducing Mortality Risk.Kundu Dibyasankha, Hazra Debapriya, Mukherjee Shayani, Jones Steven, Dey Swati, Demazumder Deeptankar