Final ID: MP606
Association Between Embolic Protection Device Use and Periprocedural Outcomes in Carotid Artery Stenting
Abstract Body (Do not enter title and authors here): Introduction: Carotid artery stenting (CAS) is increasingly used in carotid revascularization. While embolic protection devices (EPDs) are recommended during CAS to reduce the risk of periprocedural stroke and death, their actual benefit remains debated, and their use remains inconsistent in practice. We aimed to assess the association between no EPD use and in-hospital mortality, stroke, and 30-day mortality after CAS.
Methods: Patients undergoing CAS between 2015–2019 were abstracted from the Vascular Quality Initiative (VQI) registry linked with Medicare outcomes claims data and stratified by EPD use (no EPD attempted or failed vs. any EPD). Patients undergoing transcarotid artery revascularization were excluded. A 1:1 propensity score matching was performed on 29 preprocedural characteristics to compare groups. Logistic regression assessed the association between EPD use and in-hospital mortality and CAS-related stroke. Kaplan-Meier and Cox proportional hazards models evaluated 30-day mortality by EPD use. Inverse propensity weighting (IPW) was used as a sensitivity analysis.
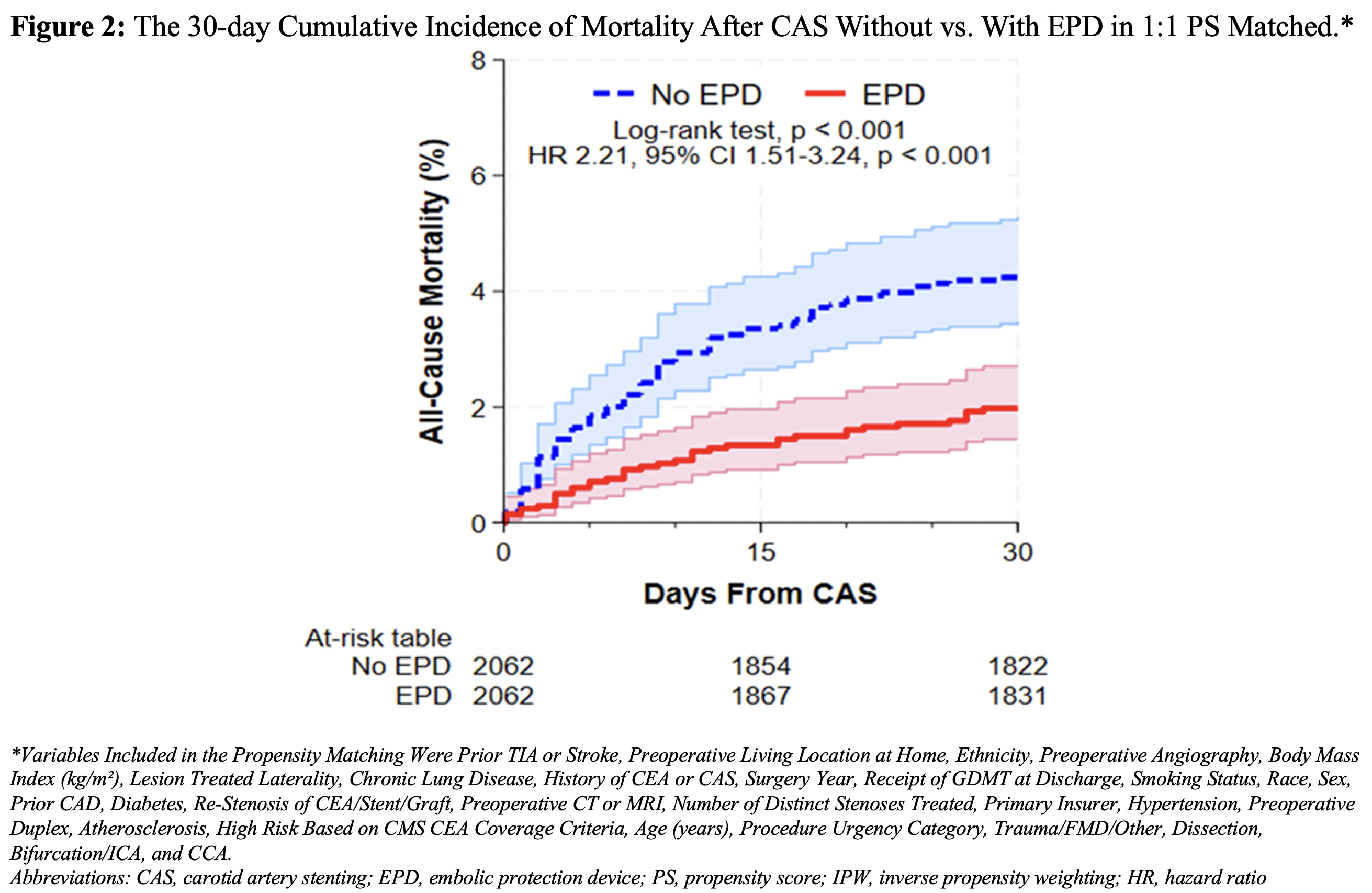
Results: Among 19,451 patients (mean age 67.1±11.7 years; 41.4% female), 2,062 individuals per group were matched (EPD vs. EPD). There was a significant association between no EPD use during CAS and the combined endpoint of in-hospital mortality or stroke (OR 1.50, 95% confidence interval [CI] 1.13–1.98, p=0.005). Individual outcome analysis demonstrated double the odds of in-hospital mortality among those in the no EPD vs. EPD group (OR 2.40, 95% CI 1.50–3.85, p<0.001), but no association with stroke (OR 1.26, 95% CI 0.91–1.75, p=0.160) (Figure 1). For 30-day mortality, the cumulative incidence was significantly higher among patients undergoing CAS without EPD (4.3% vs. 2.0%), with more than double the risk of 30-day mortality (Hazard Ratio: 2.21, 95% CI 1.51–3.24, p<0.001) (Figure 2). Results were consistent in IPW analyses.
Conclusion: Not using an EPD during CAS was associated with higher odds of in-hospital mortality or stroke, and a two-fold increase in 30-day mortality risk. As CAS becomes more common, routine EPD use should be emphasized as a quality-of-care benchmark to improve periprocedural outcomes.
Methods: Patients undergoing CAS between 2015–2019 were abstracted from the Vascular Quality Initiative (VQI) registry linked with Medicare outcomes claims data and stratified by EPD use (no EPD attempted or failed vs. any EPD). Patients undergoing transcarotid artery revascularization were excluded. A 1:1 propensity score matching was performed on 29 preprocedural characteristics to compare groups. Logistic regression assessed the association between EPD use and in-hospital mortality and CAS-related stroke. Kaplan-Meier and Cox proportional hazards models evaluated 30-day mortality by EPD use. Inverse propensity weighting (IPW) was used as a sensitivity analysis.
Results: Among 19,451 patients (mean age 67.1±11.7 years; 41.4% female), 2,062 individuals per group were matched (EPD vs. EPD). There was a significant association between no EPD use during CAS and the combined endpoint of in-hospital mortality or stroke (OR 1.50, 95% confidence interval [CI] 1.13–1.98, p=0.005). Individual outcome analysis demonstrated double the odds of in-hospital mortality among those in the no EPD vs. EPD group (OR 2.40, 95% CI 1.50–3.85, p<0.001), but no association with stroke (OR 1.26, 95% CI 0.91–1.75, p=0.160) (Figure 1). For 30-day mortality, the cumulative incidence was significantly higher among patients undergoing CAS without EPD (4.3% vs. 2.0%), with more than double the risk of 30-day mortality (Hazard Ratio: 2.21, 95% CI 1.51–3.24, p<0.001) (Figure 2). Results were consistent in IPW analyses.
Conclusion: Not using an EPD during CAS was associated with higher odds of in-hospital mortality or stroke, and a two-fold increase in 30-day mortality risk. As CAS becomes more common, routine EPD use should be emphasized as a quality-of-care benchmark to improve periprocedural outcomes.
More abstracts on this topic:
A Rare Combination: Postpartum SCAD With Fibromuscular Dysplasia
Hassan Rafla, Humayun Sara, Callejas Liam, Woosman Miranda, Nguyen-luu Tristan, Singh Anil
A Stepwise Approach to Identifying and Assessing the Content Validity of Patient-Reported Outcome (PRO) Measures for Use with Adults with Acute Heart FailureO'connor Meaghan, Loughlin Anita, Waldman Laura, Rucker Sloan, Vaghela Shailja, Kwon Namhee, Sikirica Vanja